
[ad_1]
 Glodi Muhabazi
Glodi MuhabaziBecause MPox is spreading so quickly, the World Health Organization has declared it a public health emergency of international concern, and all eyes are on the Democratic Republic of Congo, which has accounted for almost half of all recorded cases this year and more than 450 deaths.
During a visit to treatment centres in the east of the country, the BBC found that children are worst affected by the disease, which can be fatal.

“It starts with a small inflamed spot. The mother squeezes it and a watery discharge comes out. Then another one appears and before long they are all over the body,” Alain Matabaro described how his six-year-old son, Amani, became infected with mpox.
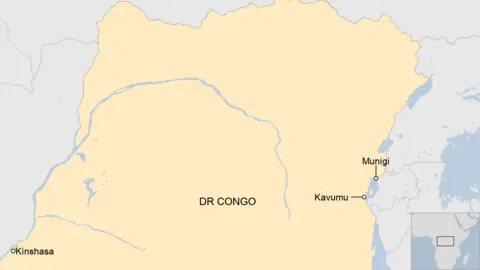
He began to recover after four days of treatment at a clinic in Muniji, near Goma, the main city in eastern Congo.
About 75 percent of the cases seen by health workers there are in patients under 10 years old, according to Dr. Pierre-Olivier Ngadjole of the charity Medair.
Young people appear to be particularly susceptible to severe effects of MPox outbreaks due to their less developed immune systems.
Dr Ngadjole also blamed overcrowding at a nearby camp for people forced from their homes by conflict in the area. He told the BBC that one of the ways MPox spreads is through very close contact, with children “always playing together. They don’t really care about social distancing”.
“You can also see families where children are even sleeping in the same bed. You can find three, four, five children. This spread is happening every day.”
Since June, Muniji’s clinic has treated 310 cases of mpox, which provides free treatment, including antibiotics for skin infections, paracetamol and safe drinking water. Currently, the clinic sees five to 10 new patients a day.
No one there has died from the disease yet, and Dr Ngadjole believes this is because people sought help early.
“I think it’s very important to provide free health care, especially in this situation… (it) means people don’t face any financial barriers and they can come to the health facility sooner.”
But at a hospital in Kavumu, 80 kilometres (50 miles) southwest of Muniji and on the other side of Lake Kivu, a different scene was unfolding.
Since June, the hospital has seen 800 patients, including eight deaths, all of whom were under the age of five.
 Glodi Muhabazi
Glodi MuhabaziTwo-year-old Ansima Kanigo contracted mpox from one of her four siblings, all of whom have the disease.
Her mother, Nzigire Kanigo, 35, had no idea what it was at first.
“This is the first time I’ve seen this happen. When my child was sick, other parents told me it could be measles but we started treating it but it didn’t work so we decided to come here.
“God bless the doctors who delivered the medicine… Three children have recovered – they have gone home. Now I have only two children in hospital. Thank God.”
Dr. Robert Musole, the hospital’s medical director, said authorities should not underestimate the outbreak.
“The situation is really serious and we are overwhelmed because our capacity is small but the demand is huge.
“The first challenge we face in responding to the epidemic is to house the patients. The second challenge is the supply of medicines, which we currently do not have.”
There are several camps in the eastern part of the Democratic Republic of Congo that house millions of people who have fled their homes due to the activities of various rebel groups in the region.
People often live in makeshift homes in poor living conditions and with poor sanitation, which is the perfect setting for porcine parvovirus to flourish.
Health workers have been visiting places such as the Muja camp near Mount Nyiragongo to educate people on what to do if they notice symptoms, such as reducing contact with others.
“This disease scares us so much, we’re afraid that all of us will get it,” said Josephine Sirangonza, who lives in the camp with her five children.
She said the government needed to provide some basic equipment to help stop the spread of the disease.
“When we see someone sick, we worry about how to protect ourselves.”
Bosco Sebuke, 52, a father of 10, had the same idea.
“We have been educated about mpox but we are still full of fear because our shelter is so crowded. Our sleeping conditions are very poor and we share bedding, so prevention is difficult and hence we are afraid,” he said.
The outbreak in eastern DRC is a new strain of mpox called Clade 1b, which has now spread to neighboring countries.
Last week, Congo’s government said it hoped vaccines would soon arrive from the United States and Japan. The country, which has not had any vaccines until now despite being the epicenter of the outbreak, has been hit hard by the pandemic.
Armani’s father, Mr. Matabaro, who is currently recovering from the cowpox virus, said he was hopeful about the news that a vaccine would be available soon.
But distribution is extremely limited, and as Dr. Ngachole said, vaccination is only one aspect of reducing the spread of the virus.
“The (easiest) action is to improve hygiene. When we improve hygiene in our homes, when we improve hygiene in our communities, it’s very easy to reduce the risk of transmission.”
Ms. Sirangonza agreed with the doctors: “Tell our leaders to send us medicines, soaps and other protective measures so that we don’t get infected.”
 Getty Images/BBC
Getty Images/BBC[ad_2]
Source link



